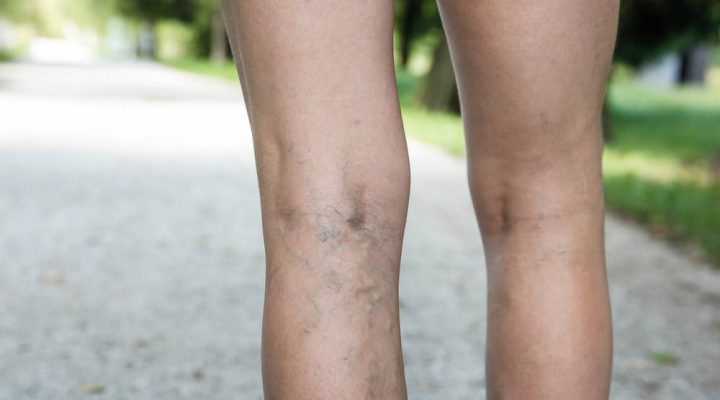
Roughly 20 per cent of Canadians experience symptoms of chronic venous disease, sometimes known as chronic venous insufficiency, each year. Since symptoms include leg pain, leg heaviness and other sensations in the lower body that are associated by many with aging, I find that my patients often don’t realize early enough they need to seek treatment.
Many of my patients are unaware of the link between these sensations they’re experiencing and chronic venous disease, so they don’t seek treatment right away. Distinguishing the symptoms of chronic venous disease from routine signs of aging is an important first step in being diagnosed and treating the condition.
This is especially crucial now that COVID-19 is affecting our lives so greatly. As we practice social isolation, we’re living through a period where it may be more difficult for some to seek in-person care from their doctors and where our usual routines have shifted dramatically from just weeks ago.
What are the early signs of chronic venous disease?
First and foremost, you’ll want to assess your legs physically. Do you have varicose or spider veins? Do your ankles or feet appear or feel swollen? Do you have spots of itchy, dry or thickened skin on your legs? These can all be potential physical manifestations of chronic venous disease. Even if you experience no pain, these are signs you should pay attention to.
The most important thing is understanding that symptoms like this aren’t just a sign of getting older. If you experience several or even just one of the below symptoms, I encourage you to start a conversation with your doctor (even via phone or web appointment):
- Leg pain (including lower leg pain and nerve pain in legs)
- Functional discomfort
- Sensation of heaviness in the legs
- Leg fatigue
- Swelling
- Burning, warmth or prickling (paresthesia)
- Night cramps
- Restless legs
- Swelling of legs
- Spider veins
- Varicose veins (in legs and feet)
- Skin changes (such as colour or thickening)
Why is it important to catch early?
Chronic venous disease is a progressive inflammatory disease caused by poor blood circulation in the legs. Most commonly affecting the lower limbs, chronic venous disease can cause physical and psychological pain and discomfort.
Chronic venous disease occurs when the vein walls or valves in the legs dilate and stop working effectively, making it difficult for blood to return to the heart from the legs. Because of this, blood begins to pool in the affected veins, which damages the valves and causes the disease to progress.
Patients often don’t come see me until their symptoms are causing them significant pain. But, since the disease is progressive, treatment is most effective when caught in the early stages. Left untreated, stagnating blood in the legs can cause further vein damage and worsen the symptoms of chronic venous disease.
Common causes and treatment of leg pain and chronic venous disease
While general leg pain can be caused by routine and strenuous daily activities like over-exercising, staying seated or standing for long periods of time and general fatigue, prolonged experience of the above symptoms may be a result of:
- Family history of the disease
- A previous leg injury, surgery or previous blood clots that caused damage to veins in the legs
- Increased pressure in the veins due to sitting or standing for long periods
- Lack of exercise
- A blood clot in a deep vein, often in the calf or thigh (deep-vein thrombosis)
- Swelling and inflammation of a vein close to the skin, often in the legs (phlebitis)
If you are a woman, pregnant or are overweight, you are also more likely to develop chronic venous disease.
The pandemic caused by the novel coronavirus this year has changed our routines in ways that may have an effect on your leg health and chronic venous disease symptoms. Many of us are isolated at home, not going outside or moving around the world as we typically do. Long periods of sitting down are more common for many of us who have transitioned to working from home or whose services have not been deemed “essential.” Any essential worker, however, may find themselves standing for long periods of time.
Both sitting and standing for prolonged periods can increase the prevalence of symptoms and worsen the condition itself. For those of us who are isolating at home, this is something we can monitor and ensure we are taking regular breaks to stand up, walk around and get blood flowing. For essential workers who have less of an option, frequently check in on yourself and be mindful of how your legs are looking and feeling.
For all of my patients suffering from chronic venous disease, I recommend overall lifestyle changes, including regular exercise to increase blood flow and weight loss for overweight people to help reduce symptoms. Some patients also find relief from their symptoms by wearing compression stockings and keeping the legs elevated.
However, for a more proactive and comprehensive approach to symptom relief, I often recommend over-the-counter medications, including venoactive products that relieve signs and symptoms of mild to moderate chronic venous disease like Venixxa.
For patients looking to be proactive in their treatment of chronic venous disease, Venixxa is made of natural ingredients extracted from immature oranges and works by improving venous tone, which helps improve blood circulation and relieve symptoms. It’s the number one over-the-counter solution recommended by doctors for treatment of chronic venous disease. If you are having difficulty accessing your doctor because of COVID-19, you can even talk to your pharmacist about it.
Assess your symptoms to know if you are at risk
If you are experiencing leg pain, heaviness or discomfort, you may be at risk of chronic venous disease. Take the veinscore assessment to understand your symptoms and learn if you are at risk.